[ad_1]
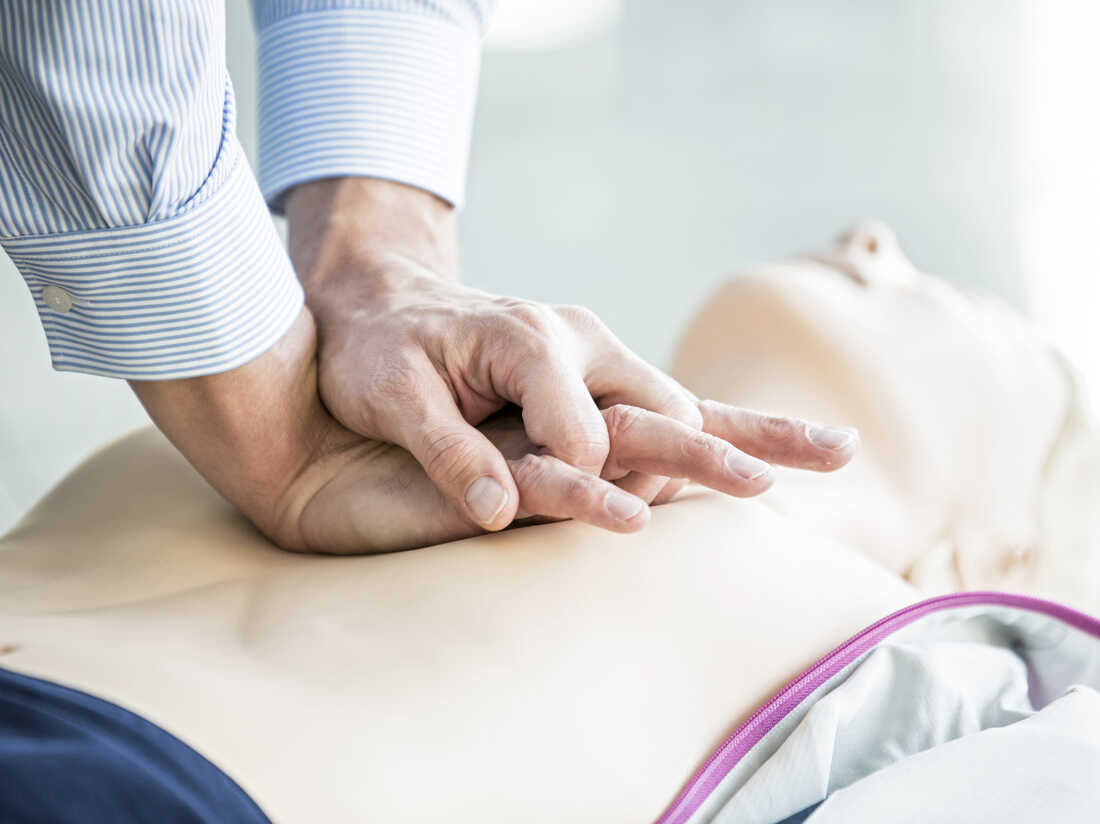
SCIENCE PHOTO LIBRARY/Getty Pictures/Science Photograph Libra

SCIENCE PHOTO LIBRARY/Getty Pictures/Science Photograph Libra
“Nurse refuses to carry out CPR,” learn the caption on an ABC newscast in California. “911 dispatcher’s pleas ignored.” A number of days earlier, an aged girl at a senior residing facility had gone into cardiac arrest. The dispatcher instructed an worker to carry out CPR, or cardiopulmonary resuscitation. However the worker refused.
“Is there anyone there that is prepared to assist this girl and never let her die?” the dispatcher stated. It made the native information, which elicited a nationwide outcry and prompted a police investigation. However the girl was already lifeless — her coronary heart had stopped. And in line with household, the girl had wished to “die naturally and with none form of life-prolonging intervention.”
So why the controversy? It comes all the way down to a widespread false impression of what CPR can, and might’t, do. CPR can generally save lives, however it additionally has a darkish facet.
The invention that chest compression might flow into blood throughout cardiac arrest was first reported in 1878, from experiments on cats. It wasn’t till 1959 that researchers at Johns Hopkins utilized the tactic to people. Their pleasure at its simplicity was clear: “Anybody, wherever, can now provoke cardiac resuscitative procedures,” they wrote. “All that’s wanted is 2 palms.”
Within the Nineteen Seventies, CPR courses had been developed for the general public, and CPR grew to become the default therapy for cardiac arrest. Flight attendants, coaches, and babysitters at the moment are typically required to be licensed. The attract of CPR is that “demise, as a substitute of a last and irrevocable passage, turns into a course of manipulable by people,” writes Stefan Timmermans, a sociologist who has studied CPR.

“That is the truest of emergencies and also you give individuals the only of procedures,” Timmermans informed me. “It appears too good to be true,” he stated, and it’s.
Many individuals be taught what they find out about CPR from tv. In 2015, researchers discovered that survival after CPR on TV was 70%. In actual life, individuals equally consider that survival after CPR is over 75%. These sound like good odds, and this may increasingly clarify the perspective that everybody ought to know CPR, and that everybody who experiences cardiac arrest ought to obtain it. Two bioethicists noticed in 2017 that “CPR has acquired a status and aura of just about mythic proportions,” such that withholding it would seem “equal to refusing to increase a rope to somebody drowning.”
However the true odds are grim. In 2010 a overview of 79 research, involving virtually 150,000 sufferers, discovered that the general fee of survival from out-of-hospital cardiac arrest had barely modified in thirty years. It was 7.6%.
Bystander-initiated CPR could improve these odds to 10%. Survival after CPR for in-hospital cardiac arrest is barely higher, however nonetheless solely about 17%. The numbers get even worse with age. A research in Sweden discovered that survival after out-of-hospital CPR dropped from 6.7% for sufferers of their 70s to only 2.4% for these over 90. Power sickness issues too. One research discovered that lower than 2% of sufferers with most cancers or coronary heart, lung, or liver illness had been resuscitated with CPR and survived for six months.
However that is life or demise — even when the chances are grim, what is the hurt in making an attempt if some will reside? The hurt, because it seems, could be appreciable. Chest compressions are sometimes bodily, actually dangerous. “Fractured or cracked ribs are the commonest complication,” wrote the unique Hopkins researchers, however the process can even trigger pulmonary hemorrhage, liver lacerations, and damaged sternums. In case your coronary heart is resuscitated, you should deal with the potential accidents.
A uncommon however notably terrible impact of CPR is known as CPR-induced consciousness: chest compressions flow into sufficient blood to the mind to awaken the affected person throughout cardiac arrest, who could then expertise ribs popping, needles coming into their pores and skin, a respiratory tube passing via their larynx.
The traumatic nature of CPR could also be why as many as half of sufferers who survive want they hadn’t acquired it, although they lived.
It isn’t only a matter of life or demise, if you happen to survive, however high quality of life. The accidents sustained from the resuscitation can generally imply a affected person won’t ever return to their earlier selves. Two research discovered that solely 20-40% of older sufferers who survive CPR had been capable of operate independently; others discovered considerably higher charges of restoration.
An excellent larger high quality of life downside is mind harm. When cardiac exercise stops, the mind begins to die inside minutes, whereas the remainder of the physique takes longer. Docs are sometimes capable of restart a coronary heart solely to seek out that the mind has died. About 30% of survivors of in-hospital cardiac arrest can have important neurologic incapacity.
Once more, older sufferers fare worse. Solely 2% of survivors over 85 escape important mind injury, in line with one research.

CPR could be dangerous not only for sufferers, but in addition for medical suppliers. In 2021, a research discovered that 60% of suppliers skilled ethical misery from futile resuscitations, and that these experiences had been related to burnout. One other research linked intrusive recollections and emotional exhaustion to troublesome resuscitations. Holland Kaplan, a doctor and bioethicist, informed me that “the unhealthy experiences far outnumber the great ones, sadly.”
She has written about performing chest compressions on a frail, aged affected person and feeling his ribs crack like twigs. She discovered herself wishing she had been “holding his hand in his final dying moments, as a substitute of crushing his sternum.” She informed me that she’s had nightmares about it. She described noticing his eyes, which had been open, whereas she was performing CPR. Blood spurted out of his endotracheal tube with every compression.
“I felt like I used to be doing hurt to him,” she informed me. “I felt like he deserved a extra dignified demise.” It is no surprise that many medical doctors are usually not keen on CPR, and select to not obtain it themselves.
The true function of CPR is to “bridge the individual to an intervention,” Jason Tanguay, an emergency doctor, informed me. “If they can not get it, or there is not one, then what’s it engaging in?” That is the essential perception that medical doctors have and most others do not. CPR is a bridge, nothing extra. Generally it spans the gap between life and demise, if the trigger could be shortly reversed, and if the affected person is pretty younger and comparatively wholesome. However for a lot of that distance is simply too nice. “The act of resuscitation itself can’t be anticipated to treatment the inciting illness,” the Hopkins researchers wrote in 1961.
A affected person with terminal most cancers who’s resuscitated will nonetheless have terminal most cancers. In these instances, essentially the most humane method could also be to ease the ache of the dying course of, relatively than construct a bridge to nowhere.
How can physicians assist sufferers make these selections upfront? A part of it’s schooling. Research have discovered that half of sufferers modified their needs once they discovered the true survival charges of CPR, or after watching a video depicting the truth of CPR.
One other half is communication. In response to one survey, 92% of People consider it is vital to debate end-of-life care, however solely 32% have executed so. Physicians (or sufferers) ought to provoke these conversations early, particularly for many who are aged or have power medical issues, in order that their needs are recognized upfront in the event that they undergo a cardiac arrest.
Language issues too. Docs typically ask if sufferers “need every little thing executed” if their coronary heart stops. However that places a burden on sufferers and households. “Who needs to really feel like they do not need every little thing executed for his or her beloved one?” Kaplan says. As an alternative, if CPR would possible be futile, medical doctors might advocate “permit pure demise” as a substitute of “don’t resuscitate,” suggests Ellen Goodman, director of a non-profit that encourages end-of-life conversations.
“Give individuals one thing they will say sure to,” she informed me. Physicians have the information and expertise to information sufferers in selecting measures they could profit from, declining those who could hurt, and aligning interventions with their needs and values. An important factor, as a substitute of at all times taking motion, is to ask.
Clayton Dalton is a author in New Mexico, the place he works as an emergency doctor.
[ad_2]
Source link















